I found out we were expecting our fourth child in January 2011 at about two weeks. Due to my history, the doctor wanted to see me ASAP. I went in at six weeks along. Everything looked great. Then around eight weeks I became very sick I was in and out of hospital for IV fluids and medicines.
At twelve weeks along, on a Wednesday I had a home nurse come out to show me how to use the Zofran pump. (For those that don't know this is a slow steady flow of medicine running all the time to help with the sickness.) I had lost 20lbs. A small needle was put through my tummy that delivered the medicine.
The next day I was at work. I worked with preschool kids at my church. I thought I had peed myself as it tends to happen in pregnant women. But little did I know what was about to happen. I had started bleeding everywhere. I was rushed via ambulance to the nearest hospital. I thought I was losing the baby. The doctor wasn't sure if the baby would make it let alone myself. I was diagnosed with Subchorinic Hematoma (SCH).
I was followed very closely until my thirty week point by my OB and a specialist. I had two blood clots in my uterus along side of the baby. They cleared up at twenty-eight weeks. I was told all was good the baby was large and growing fine I came off bed rest around thirty-two weeks when I had the finally all clear and my baby boy was doing good. So our fear of premature birth was gone. No nicu stay was going to happen.
We were all good right there right up until inducement day. My husband and I had this really bad feeling. My thoughts were... I don't want to have this baby. Something is wrong. We got to the hospital at 7:00 and he was here at 10:28am weighing 10lbs 4 ounces and 22 inches long. He was blue and not breathing.
No one would tell me what was wrong. They all turned from me and were crying. I had been given the chance to hold him but said no cause I figured I'd get to hold him after he was cleaned up like I did with my others. We didn't know he was sick.
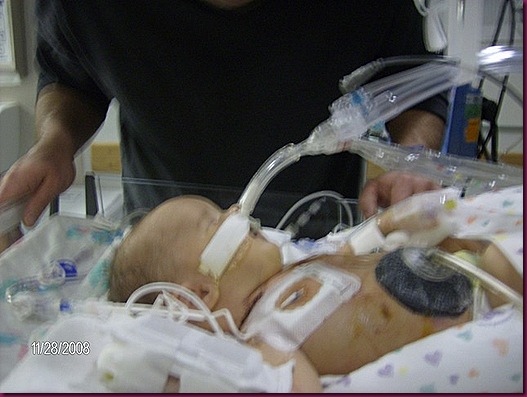
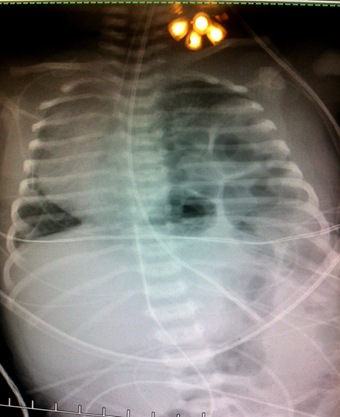
They took him out in the incubator. They tubed him and came in and told me he had aspirated. I was ok with that. I knew what that was and it would just be a couple days in nicu. Then came the bad news, the doctor said "I have some upsetting news, Your baby has congenital diaphragmatic hernia." I said, Do what!!" And then he explained that he had a hole in his diaphragm and his organs weren't in the right spot.
His hospital keep getting changed due to them not having the right equipment like the ECMO. We finally had a hospital for him to go to. The place I delivered didn't even have a nursery for babies. He was transported by the angel team that evening by the time they got there had him all hooked up and sedated. They told me to say my good byes because they didn't know if he would make the transfer or thru the night. I couldn't go because I had just delivered a baby. I told my doctor I wanted out first thing in morning and I was. With a cracked tailbone I made my way down to Children's hospital, a an 2 hours drive away.
Andy was on a vent that was breathing for him and on a lot of pain medicines.
Things are hard to recall everything as I was in shock, mad, upset and in a lot of pain both mentally and physically. I didn't understand why I was told everything was finally ok and it wasn't. From what all I can remember he only had his intestine in his chest he had a 30% hole they said he has stitches mess and the Gortex patch. He had pulmonary hypertension. He was born on a Monday had his repair on Friday. It took couple hours at least 5 hours cause I had to pump twice why waiting. I was so worried about going to pump in case the call came in and something happened.
All went well he had it done laparoscopically. He has about a three inches scar on his back and a couple small holes under his arm by his shoulder, where he had a chest tube. He had fluid in his lungs it was a nasty color when it drained out. We were told he would come home until Christmas then it was Thanksgiving it just keep going back and forth.
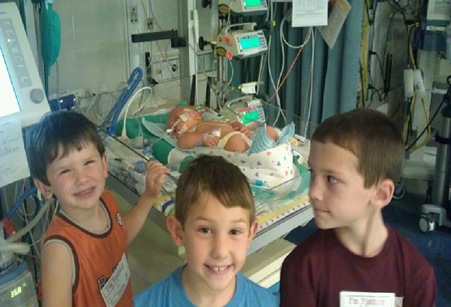
We still had three other boys to take care of and tell them what was going on it was very hard they didn't get to see their baby brother until he was almost a week old after surgery.
We were scared that he wasn't going to make it. He develop some kind if infection so they gave him high dose of antibiotics.
It was a roller coast. His vent would be turned down and he would be doing good. We would get home and call to check on him and he wasn't doing good and had to turn the ventilator back up. I finally got to hold him at nine days old. The next day he came off the ventilator.
Then came the feeds, he wouldn't eat for the nurses but would for me I wasn't allowed to stay with him at night so during the daytime he would take a bottle and at night would be feeding tube.
He was still having trouble with his breathing and heart rate going up when he would eat. After two weeks of feeds and finally gaining weight, they allowed him to breastfeed and he had a hard time with it. He couldn't breath so it was back to the bottle which at that time I didn't care I just wanted him to eat and come home.
Two weeks old they moved him to another room where I could stay with him. He came home right at a month old. He needed no oxygen! He did need reflux medicine and had to sleep upright cause of reflux and sometimes he would stop breathing if laying flat. He develop another hernia which they are watching now closely. He's one and is into everything. We still have problems with him not wanting to eat or choking on his bottles. He has immature swallowing food allergies and they keep finding more things wrong as he grows. He's a happy sweet loving little boy.
~Amber Parker (Andy's Mom)










.jpg)
.jpg)
+final.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)